By Calli | Licensed Chiropractor & Esthetician | May 3, 2026
Most patients who walk into my Los Angeles clinic and tell me “I have sciatica” do not actually have sciatica. They have something that hurts in the same general area — a tight piriformis, an irritated SI joint, a referred pattern from the hip — and have used the word as shorthand. After 20 years of treating this presentation, I can usually tell within the first 60 seconds of an exam whether the nerve is genuinely involved. True sciatica has a specific signature, and once you know what to look for, the difference is hard to miss.
It matters which one you have because the fix is different. Stretching a tight glute will not calm an irritated nerve root. Decompressing a nerve will not loosen a fused-feeling hip. This article walks through what sciatica actually is, what causes it, how to separate it from the imposters, and the protocol I have refined over two decades of treating LA patients to get them out of pain at home.
Quick Summary
Sciatica is not a disease. It is a symptom — pain that travels along the sciatic nerve, almost always caused by something compressing or irritating one of the lower spinal nerve roots. The five common causes are a herniated or bulging disc, piriformis syndrome, spinal stenosis, pregnancy-related compression, and prolonged sitting. Most cases settle within six weeks of the right home protocol; a small minority need imaging and hands-on care.
In This Article
1. What sciatica actually is — and what it is not
2. What actually causes sciatica pain
3. How to tell sciatica from hip pain or lower back pain
4. How to relieve sciatica pain at home (and when to see a chiropractor)
WHY TRUST THIS ARTICLE
Written by Calli — a licensed Doctor of Chiropractic (DC) and Licensed Esthetician (LE) in Los Angeles with 20 years of clinical experience. Sciatica is one of the conditions I assess most often in clinic. Every claim here reflects current orthopedic literature combined with thousands of hours of hands-on practice using techniques like the straight leg raise test, slump test, McKenzie assessment, and Cox flexion-distraction. Educational content, not a substitute for an exam.
1. What Sciatica Actually Is — and What It Is Not
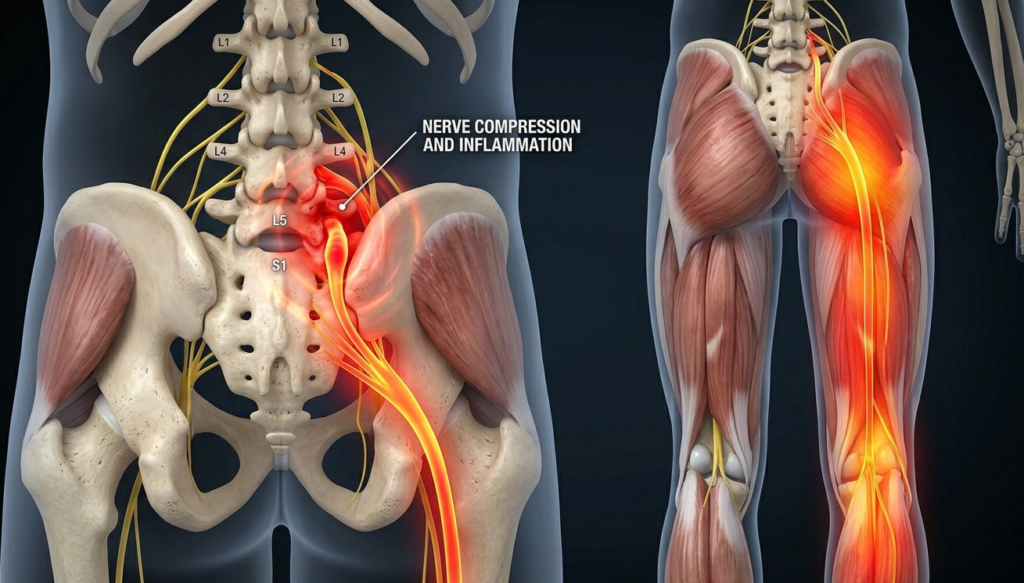
The sciatic nerve is the largest nerve in the human body. It is roughly the diameter of a pencil at its origin, and it forms from five nerve roots that exit the lower spine between the L4 vertebra and the S3 sacral segment. Those roots merge into one thick nerve that runs through the buttock, down the back of the thigh, behind the knee, and branches into the lower leg and foot. When you feel pain that travels from the lower back into the buttock and down the leg, you are following the path of that nerve.
The sciatic nerve in plain English
Think of the sciatic nerve as the main electrical cable that powers your leg. The lower spine is the breaker box. Anything that squeezes, pinches, or chemically irritates one of the five roots in that breaker box can light up the entire cable downstream. In my 20 years of practice in Los Angeles, the most common patient pattern I see for true sciatica is a 35–55-year-old desk worker who first noticed the symptom after a long flight, a weekend move, or several days of unusually heavy sitting. The pain shows up in the calf or foot — nowhere near where the actual problem lives.
Sciatica is a symptom, not a diagnosis
This is the single most important point in the entire conversation, and it is the first thing I clarify with every new patient. Sciatica is not a condition you are diagnosed with the way you would be diagnosed with diabetes. It describes a pattern of pain. The diagnosis is what is causing the pattern. When I take a new sciatica history, my goal is not to confirm “you have sciatica” — my goal is to identify which structure is irritating which root, because that single answer determines whether the patient needs disc-style decompression, soft-tissue release of the piriformis, or stenosis-style flexion exercises. Three completely different protocols, one shared label.
2. What Actually Causes Sciatica Pain
Five causes account for the overwhelming majority of cases I see in my LA clinic. They are not equally common across age groups, and a careful history usually narrows the list within the first few minutes of intake.
A herniated or bulging disc
This is the textbook cause and the most common one I treat in adults under fifty. The discs between your vertebrae are essentially shock-absorbing pads with a tough outer ring and a softer gel-like center. When the outer ring weakens, the inner gel can push outward (a bulge) or push through (a herniation), and the resulting bump presses on the nerve root that exits next to it. The hallmark in my exam room: sharp, leg-dominant pain that gets worse with bending forward, sneezing, sitting in a soft chair, or putting on socks. When I perform the McKenzie repeated-extension assessment on these patients, the leg pain often centralizes back toward the spine within 10 repetitions — that is the single best in-clinic predictor that conservative care will work.
Piriformis syndrome
The piriformis is a small, deep muscle in the buttock. In a meaningful percentage of people the sciatic nerve runs directly under it, and in some it actually runs through it. When the piriformis is overworked or held tight for hours of sitting, it compresses the nerve. The pain is usually buttock-dominant rather than leg-dominant, worse with sitting, eased by walking. It mimics disc-driven sciatica almost perfectly, and over 20 years I have seen it misdiagnosed as a disc more times than I can count. In my office I confirm it with a combination of the FAIR test and direct palpation through the gluteal mass — if pressing the piriformis reproduces the leg pain, the diagnosis is usually clear.
Spinal stenosis, pregnancy, and prolonged sitting
In the LA patients I see over fifty, the most common cause shifts toward spinal stenosis — an age-related narrowing of the canal where the nerve roots travel. The pain pattern is different: worse with standing and walking, better with sitting or leaning forward. In pregnancy, the growing uterus and the postural changes that come with it compress the nerve roots and irritate the piriformis. And in everyone else, the silent factor is hours of sitting. The longer the lower back is held in flexion, the more pressure ends up on the lumbar discs — which is why I cover the upstream mechanics in detail in my guide on what sitting all day does to your spine.
3. How to Tell Sciatica From Hip Pain or Lower Back Pain
Most of the patients who walk into my LA office convinced they have sciatica actually have one of two impostors: hip-driven referred pain or pure lower back pain that has not crossed into the leg. The differences are real and you can usually identify them at home in about a minute.
The classic sciatica pattern
Real sciatica almost always travels below the knee. The pain follows a line — back of the thigh, behind the knee, into the calf or the outside of the lower leg, sometimes into the foot. It is often described as electric, burning, or shooting. Numbness, tingling, or weakness in the leg or foot points strongly toward nerve involvement. In my clinical experience, if symptoms stay in the buttock and never cross the knee, the diagnosis is rarely true sciatica — and the treatment changes accordingly.
When the pain is actually hip-driven
Hip joint problems — impingement, labral irritation, early osteoarthritis — refer pain into the buttock and groin in a pattern that can feel almost identical to sciatica. The give-aways I look for in my exam: pain provoked by hip movement (squatting, getting in and out of a car), leg pain that stops at the knee, and no numbness or tingling. When I perform the FADIR test (flexion-adduction-internal rotation) and it reproduces a familiar pinch in the front of the hip, I am thinking impingement, not nerve compression. I walk through that mechanism in my article on hip pinching when you sit.
A 30-second home test (the slump test, simplified)
The slump test is one of the most useful tools I run in clinic, and a simplified version works at home. Sit on the edge of a firm chair with your back straight. Slowly straighten one knee until the leg is almost parallel to the floor, then point your toes up toward your face. If straightening the knee and pulling the toes back reproduces a sharp electric pain that travels down the back of the thigh into the calf, that is a positive home version of the slump test — a strong indicator of nerve-root irritation. If the same movement only produces hamstring tightness or hip pinching, the source is muscular or joint-driven, not neurological. This is not a diagnosis, but it is the single most useful self-screen I teach my Los Angeles patients before their first visit.
4. How to Relieve Sciatica Pain at Home (and When to See a Chiropractor)
For the majority of cases I see, the right combination of movement, decompression, and time will resolve sciatica without any clinical intervention. The trick is doing the right things and avoiding the wrong ones — which most patients I see have backwards on their first visit.
3 movements that actually help
First, prone press-ups (the McKenzie press-up). Lie on your stomach, place your hands under your shoulders, and gently push your chest up while keeping your hips on the floor. Hold for two seconds, lower, repeat ten times. This decompresses the lower discs and, in my experience, often relieves nerve pressure within the first two or three sets when the cause is disc-driven. Second, the supine figure-four. Lie on your back, cross one ankle over the opposite knee, and pull the bottom thigh toward your chest. This unloads the piriformis. Third, walking. Five to ten minutes every two hours, easy pace, ideally outdoors. Walking is almost universally the most underused recovery tool in the patients I see.
3 stretches that make sciatica worse
Aggressive seated forward folds, deep hamstring stretches with a rounded back, and any flexion-dominant yoga position. All three increase the pressure on the lumbar discs and the irritated nerve root. The instinct when something hurts is to stretch it; with disc-driven sciatica, my clinical recommendation is the opposite. If forward bending makes the pain worse during your home self-check, that movement is what was causing it in the first place — and it needs to come out of your routine until the nerve quiets.
When to escalate to a chiropractor or physical therapist
Pain that has not improved after two weeks of consistent self-care, progressive weakness in the leg or foot, loss of bowel or bladder control, or saddle-area numbness. The last two are emergencies and warrant immediate evaluation. Otherwise, an in-clinic assessment will pinpoint which root is involved and what specific protocol fits your case. In my LA office, the disc-driven cases respond best to Cox flexion-distraction combined with a graded McKenzie program. The piriformis-driven cases respond best to a combination of instrument-assisted soft tissue mobilization (IASTM), manual myofascial release, and a daily home stretch sequence. Imaging is reserved for the cases that do not respond — not the starting point.
Calli’s Clinical Note
In 20 years of running an LA clinic, the patients who recover from sciatica fastest are not the ones who push through the pain or the ones who lie completely still. They are the ones who follow a simple two-rule protocol: stop doing the position that triggers the pain, and walk a little every couple of hours. That single combination — remove the provocateur, restore gentle movement — outperforms almost every fancy intervention I have ever tried. The patients who add Cox flexion-distraction and a daily McKenzie press-up sequence usually cut their recovery time in half again.
The Bottom Line
Sciatica is not a diagnosis — it is a description of pain along a specific nerve. Identify which of the five common causes is yours, remove the position that provokes it, add gentle decompression and walking, and most cases improve within a few weeks. If yours does not, or if any red flag appears, get evaluated rather than guessing.
Related Reading
Why Sitting All Day Is Destroying Your Spine — A Chiropractor’s Essential Desk Stretching Protocol — the upstream cause of most adult-onset sciatica I see in my LA practice, and the one habit that resets the entire chain.
Herniated Disc vs Bulging Disc: A Chiropractor Explains the Difference
A bulge and a herniation are not the same thing — and the difference changes everything about how it should be treated. Next article walks through both, and what to do for each.
— Calli
DC, LE | Licensed Chiropractor & Esthetician | Aligning the body, glowing the skin, one habit at a time.
Medical disclaimer: This article is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Sciatica can be caused by serious conditions including disc herniation with progressive neurological deficit and, rarely, cauda equina syndrome — an emergency. If you experience progressive leg weakness, loss of bladder or bowel control, or saddle-area numbness, seek immediate medical care. Always consult a licensed healthcare provider for an evaluation specific to your case.
Pingback: What’s the Best Sleeping Position for Back Pain? A Chiropractor’s Honest Answer – calliglowalign.com